Risk Factors
Multiple risk factors have been identified for aortic dissection. These include lifestyle and genetic factors. This page explains more about these risk factors.
General Risk Factors
- Aneurysm – a bulge in the aorta (which may be genetic, as with aortic dissection itself). These are more common with advancing age.
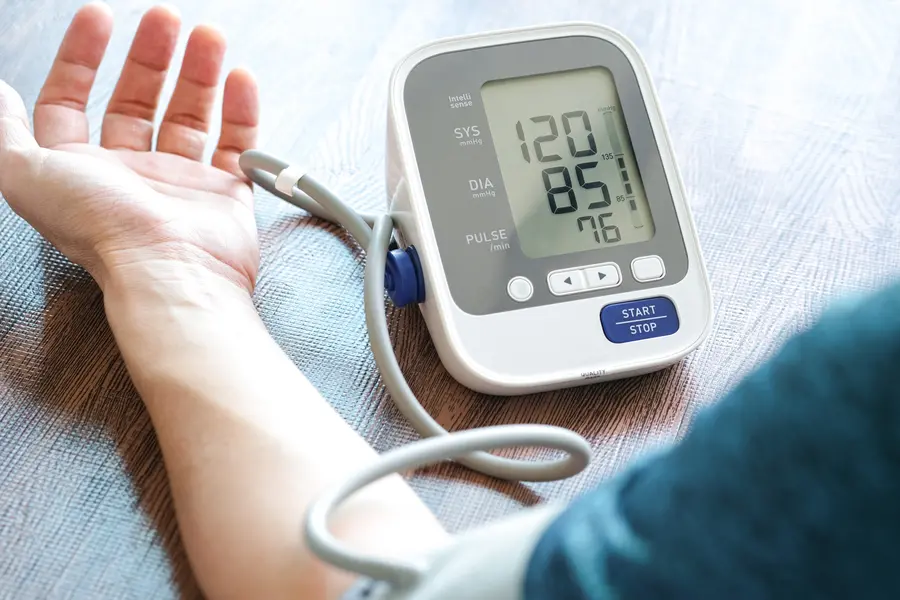
- High blood pressure – high blood pressure directly exerts excessive force on the aorta, forcing it to stretch.
- Bicuspid aortic valve (BAV) – the aortic valve is found between the heart and aorta. It opens to let the blood out and then closes to stop blood leaking back into the heart. BAV is when the aortic valve, which normally has three leaflets (‘tricuspid’), has only two leaflets (‘bicuspid’). This can cause the valve to leak or become narrow. A ‘murmur’ may be heard through a stethoscope if this is the case, which is the sound of blood flowing backwards through the valve after it has closed. BAV affects 1-2% of the population. The risk of aortic dissection with a BAV is difficult to quantify and research on this is ongoing. However, AD patients with BAV tend to be younger than those with a tricuspid valve, are less likely to have high blood pressure and may have other aortic disease prior to dissection (either undiagnosed or diagnosed).
- Trauma – trauma such as a car crash can cause an aortic dissection, though normally only if the aorta already has some weakness. For severe trauma such as this, the aorta can also rupture.
- Illegal/illicit drugs – cocaine usage is a known risk factor for aortic dissection.
- Atherosclerosis – in a similar way to building up plaque (fatty deposits) inside a person’s coronary arteries, plaque can build up on the inside of the aorta and accelerate degradation of the aortic tissues. Plaque is often due to risk factors such as smoking, diabetes, high blood pressure and high cholesterol. A particular risk is that of a ‘penetrating atherosclerotic ulcer’ or PAU. This is an ulcer which usually forms beneath plaque and penetrates into the aortic wall, causing a weak spot in the wall. This can (but may not) initiate an aortic dissection. Up to 7% of aortic dissections are due to a PAU.
- Weight lifting and other sports – weight lifting can induce extreme blood pressure peaks, particularly if the person does not breathe properly or holds their breath. On its own, weight lifting should not cause an aortic dissection but can precipitate one if there is already an aortic weakness. A minority of dissections are precipitated by other sports, including contact sports, typically involving elevated blood pressure, heavy contact, turning or stretching. Again, such activities should not cause an aortic dissection but can initiate one if there is an aortic weakness.
- Pregnancy – pregnancy is also a risk factor for aortic dissection. Carrying a baby increases stress on the mother’s cardiovascular system and causes hormonal changes. Some of the drugs that are used around the time of delivery can also increase the risk. High blood pressure in pregnancy or pre-eclampsia will increase this risk.
Genetic Risk Factors
In addition to the general risk factors, aortic disease and dissection can run in families and hence can be called 'familial' or 'heritable' (inherited) conditions. In these cases, the disease is caused by faulty genetic mutations. Mutations are very small changes in the genetic makeup of cells which make up our bodies, and can lead to changes in the cell and tissue properties. Mutations are sometimes called variants. When these mutations affect the aorta, they fall into one of two categories.
- Syndromic – ‘syndromic’ means that the patient will usually have a number of typical features together, i.e. a syndrome. These can include tall stature, long limbs, curvature of the spine, a particular facial appearance, or ‘tortuous’ blood vessels. Not everyone with a syndrome will display all of these. The most common syndromes are Marfan, Loeys-Dietz, and Ehlers-Danlos Syndromes. Turner’s Syndrome is another condition, which is confined to women. It can lead to bicuspid aortic valve and aortic dissection. Turner’s syndrome is often associated with short stature and other features (see NHS websites). All of these syndromes are sometimes referred to as ‘connective tissue disorders’ or CTDs, as it is the connective tissues of the body that are affected, leading to the features listed. As well as the syndromic features noted, all these genetic disorders also typically weaken the aortic tissues and predispose a person to aortic dissection. Overall, somewhere between 5% and 20% of aortic dissections are associated with CTDs. Aortic dissections due to CTDs tend to occur at an earlier age (typically age 40-50) than for other types. Where a patient has one of these syndromes, the culprit gene can usually be identified.
- Non-Syndromic – in non-syndromic cases the condition runs in the family but there are none of the other physical features described in the syndromes above. Though these cases clearly have a genetic basis which can sometimes be identified through testing, it may not be possible to find a culprit gene in every case.
In both groups, the faulty genetic mutation is usually inherited and when that is so, it occurs in such a way that parents have a 50:50 chance of passing it on to each of their children. It affects males and females equally and does not skip a generation. However, some members of the family may be more severely affected than others. In a very small minority of cases, the person affected will not have inherited the condition from anyone, but will be the start of a family trait.
Genetic testing is particularly relevant to those dissecting before they are 60 years old. Here are the current NHS criteria qualifying patients and relatives for genetic testing.


